IMPACT OF MULTIDISCIPLINARY TEAM IMPLEMENTATION ON SURVIVAL AND QUALITY OF CARE INDICATORS IN METASTATIC NON-SMALL CELL LUNG CANCER: A RETROSPECTIVE SINGLE-CENTER COHORT STUDY IN THAILAND
DOI:
https://doi.org/10.55374/jseamed.v10.280Keywords:
metastatic non-small cell lung cancer, multidisciplinary team, molecular testing, time to treatment initiation, real-world evidenceAbstract
Background: In resource-limited settings such as Thailand, metastatic non-small cell lung cancer (NSCLC) outcomes are adversely affected by fragmented care and delayed diagnosis and treatment. At the same time, the impact of the multidisciplinary team (MDT) remains uncertain.
Objectives: The study aimed to evaluate the effect of MDT implementation on overall survival (OS), time to treatment initiation, and molecular testing rates in patients with metastatic NSCLC at a Thai tertiary cancer center.
Methods: This retrospective study included patients with newly diagnosed metastatic NSCLC treated between 2018 and 2023. Patients were categorized according to whether their treatment was planned before or after the establishment of MDT in 2020. Baseline characteristics, molecular testing rates, and treatments were compared. The OS was the primary endpoint and was analyzed using Kaplan–Meier methods and multivariable Cox proportional hazards models.
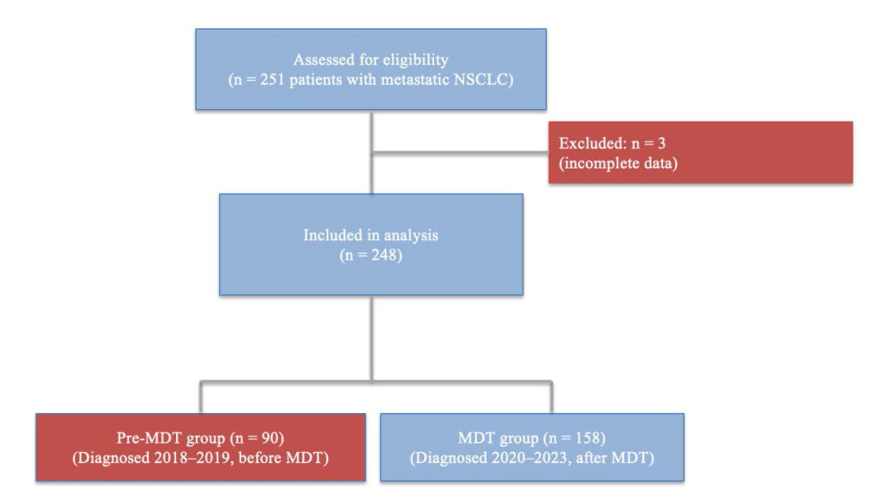
Results: Among 248 eligible patients, 158 were managed in the MDT era and 90 in the pre-MDT era. Patients in the MDT group demonstrated a trend toward earlier treatment initiation (median 1.21 vs 1.52 months; approximately 33.8 vs 42.5 days; p = 0.18) and numerically higher EGFR testing rates (66.89 % vs 56.79 %; p = 0.09), whereas ALK testing was significantly more frequent in this group (32.10 % vs 18.03 %; p = 0.04). There was no statistically significant difference in OS between groups (median OS 10.44 vs 15.73 months; adjusted HR 1.25 (95% CI 0.94–1.67; p = 0.12). After adjustment for possible confounders, age ≥ 65 years (HR 2.09; 95% CI 1.07-4.11; p = 0.03), male sex (HR 3.90; 95% CI 1.28-11.88; p = 0.02), ECOG performance status ≥2 (HR 3.58; 95% CI 1.34-9.59; p = 0.01), non-adenocarcinoma histology (HR 12.30; 95% CI 1.44-104.44; p = 0.02), and multiple metastatic sites (HR 2.73; 95% CI 1.22-6.14; p = 0.01) were independently associated with poorer survival.
Conclusion: MDT implementation was associated with earlier treatment initiation and higher rates of molecular testing in metastatic NSCLC. Although no significant survival benefit was observed, MDTs remain important in real-world practice.
Downloads
Metrics
References
Ferlay J, Colombet M, Soerjomataram I, Parkin DM, Piñeros M, Znaor A, et al. Cancer statistics for the year 2020: An overview. Int J Cancer 2021: 48: 778-89. DOI: https://doi.org/10.1002/ijc.33588
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide. CA: Cancer J Clin 2021; 71: 209-49. DOI: https://doi.org/10.3322/caac.21660
Reungwetwattana T, Oranratnachai S, Puataweepong P, Tangsujaritvijit V, Cherntanomwong P. Lung cancer in Thailand. J Thorac Oncol 2020; 15: 1714-21. DOI: https://doi.org/10.1016/j.jtho.2020.04.024
Montagne F, Guisier F, Venissac N, Baste JM. The role of surgery in lung cancer treatment: Present indications and future perspectives—state of the art. Cancers (Basel) 2021; 13: 3711. DOI: https://doi.org/10.3390/cancers13153711
Vinod SK, Hau E. Radiotherapy treatment for lung cancer: Current status and future directions. Respirology 2020; 25(Suppl 2): 61-71. DOI: https://doi.org/10.1111/resp.13870
Miller M, Hanna N. Advances in systemic therapy for non-small cell lung cancer. BMJ 2021; 375: n2363. DOI: https://doi.org/10.1136/bmj.n2363
Didkowska J, Wojciechowska U, Mańczuk M, Łobaszewski J. Lung cancer epidemiology: Contemporary and future challenges worldwide. Ann Transl Med 2016; 4: 150. DOI: https://doi.org/10.21037/atm.2016.03.11
Goldstraw P, Chansky K, Crowley J, RamiPorta R, Asamura H, Eberhardt WE, et al. The IASLC Lung Cancer Staging Project: Proposals for revision of the TNM stage groupings in the forthcoming (eighth) edition of the TNM classification for lung cancer. J Thorac Oncol 2016; 11: 39-51. DOI: https://doi.org/10.1016/j.jtho.2015.09.009
Hung HY, Tseng YH, Chao HS, Chiu CH, Hsu WH, Hsu HS, et al. Multidisciplinary team discussion results in survival benefit for patients with stage III non-small-cell lung cancer. PLoS One 2020; 15: e0236503. DOI: https://doi.org/10.1371/journal.pone.0236503
Saeteng S, Chewaskulyong B, Charoentum C, Lertprasertsuke N, Euathrongchit J, Tajarernmuang P, et al. The impact of a multidisciplinary team conference on non-small cell lung cancer care: Time barriers and longterm outcomes. J Clin Med 2024; 13: 5276. DOI: https://doi.org/10.3390/jcm13175276
Pan CC, Kung PT, Wang YH, Chang YC, Wang ST, Tsai WC. Effects of multidisciplinary team care on the survival of patients with different stages of non-small cell lung cancer: A national cohort study. PLoS One 2015; 10: e0126547. DOI: https://doi.org/10.1371/journal.pone.0126547
Bandidwattanawong C, Kerkarchachai G. The benefits of G8 and VES-13 geriatric screening tools for older patients with advanced lung cancer. J Geriatr Oncol 2022; 13: 1256-59. DOI: https://doi.org/10.1016/j.jgo.2022.04.016
Dall’Olio FG, Maggio I, Massucci M, Mollica V, Fragomeno B, Ardizzoni A. ECOG performance status ≥2 as a prognostic factor in patients with advanced non-small cell lung cancer treated with immune checkpoint inhibitors-A systematic review and meta-analysis of real world data. Lung Cancer 2020; 145: 95-104. DOI: https://doi.org/10.1016/j.lungcan.2020.04.027
Le Caer H, Borget I, Corre R, Locher C, Raynaud C, Decroisette C, et al. Prognostic role of a comprehensive geriatric assessment on the management of elderly patients with advanced non-small cell lung cancer (NSCLC): a pooled analysis of two prospective phase II trials by the GFPC Group. J Thorac Dis 2017; 9: 3747-54. DOI: https://doi.org/10.21037/jtd.2017.09.51
Kowalczyk A, Jassem J. Multidisciplinary team care in advanced lung cancer. Transl Lung Cancer Res 2020; 9: 1690-98. DOI: https://doi.org/10.21037/tlcr.2019.11.33
Blackhall F, Thatcher N, Booton R, Kerr K. The impact on the multidisciplinary team of molecular profiling for personalized therapy in non-small cell lung cancer. Lung Cancer 2013; 79: 101-3. DOI: https://doi.org/10.1016/j.lungcan.2012.10.016
Taberna M, Gil Moncayo F, Jané-Salas E, Antonio M, Arribas L, Vilajosana E, Peralvez Torres E, Mesía R. The multidisciplinary team (MDT) approach and quality of care. Front Oncol 2020; 10: 85. DOI: https://doi.org/10.3389/fonc.2020.00085
de Castro G Jr, Souza FH, Lima J, Bernardi LP, Teixeira CHA, Prado GF; Grupo Brasileiro de Oncologia Torácica (GBOT). Does multidisciplinary team management improve clinical outcomes in NSCLC? A systematic review with meta-analysis. JTO Clin Res Rep 2023; 4: 100580. DOI: https://doi.org/10.1016/j.jtocrr.2023.100580
Williams GJ, Thompson JF. Management changes and survival outcomes for cancer patients after multidisciplinary team discussion: a systematic review and meta-analysis. Cancer Treat Rev 2025; 139: 102997. DOI: https://doi.org/10.1016/j.ctrv.2025.102997
Ciccolella TJ, Walker A, Ashkezari AD, Huang X, Hong Y, Sangal A, et al. Introduction of multidisciplinary team at a comprehensive cancer center affects time to tissue diagnosis and definitive treatment. Ann Lung Cancer 2025; 5 96-105.
Castro G Jr, Souza F, Bernardi LP, Teixeira CH, Prado G. The impact of multidisciplinary teams on the diagnosis and staging of non-small cell lung cancer: a systematic review and meta-analysis. J Thorac Oncol 2023; 18(3 Suppl 2): S27. DOI: https://doi.org/10.1016/j.jtho.2023.01.073
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Journal of Southeast Asian Medical Research

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







