EVALUATING AN INNOVATIVE CO-CREATION MODEL FOR TEACHING AND LEARNING IN COMMUNITY MEDICINE
DOI:
https://doi.org/10.55374/jseamed.v10.268Keywords:
student co-creation, community medicine, medical education, active learning, learner engagementAbstract
Background: As preventive medicine gains importance, healthcare professionals must be equipped with competencies in community health promotion and engagement. To strengthen these skills, a student co-creation model was introduced in the “Introduction to Community Medicine” course at Phramongkutklao College of Medicine, Thailand. Third-year medical students were divided into ten groups and tasked with designing and delivering peer-teaching sessions on public health topics, positioning them as both learners and educators. Despite its growing recognition, co-creation in community medicine remains underexplored, particularly in settings where students assume dual roles as teachers and learners.
Objectives: This study evaluated students’ perceptions of the co-creation model and its performance in examinations compared with traditional lecture-based learning in community-oriented medical education.
Methods: This descriptive study compared examination outcomes between the 2022 lecture-based cohort and the 2023 co-creation cohort. Examination data were analyzed using descriptive statistics and measures of variability. Student perceptions were collected through an anonymous survey comprising five-point Likert-scale items, open-ended questions, and a multiple-choice recommendation item, yielding an 80% response rate (N = 95).
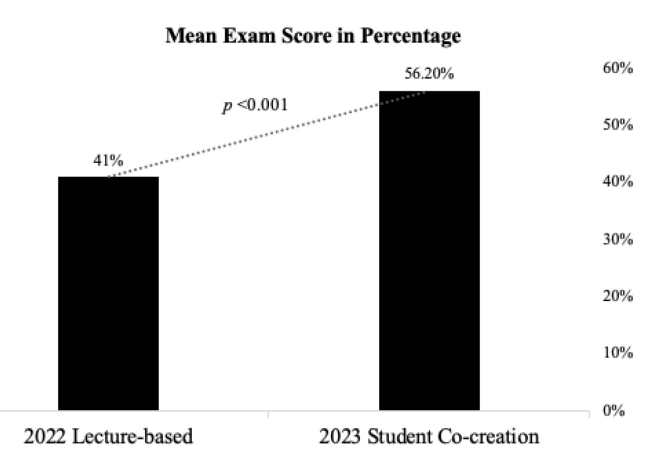
Results: Students reported positive perceptions of the co-creation experience, describing it as engaging and meaningful for learning through teaching. Reported learning related experiences included communication skills, teamwork, creativity, and confidence in explaining public health concepts. Challenges like time constraints and uneven workload distribution among group members are also reported. A majority of respondents indicated that they would recommend continuing the co-creation approach. Examination scores differed between the 2022 and 2023 cohorts, with mean scores of 41.0% and 56.2%, respectively. Score variability, expressed as the coefficient of variation, was 21.6% in 2022 and 17.5% in 2023. These results are presented descriptively, and no causal inferences can be drawn from this comparison.
Conclusion: Student co-creation was associated with positive learning experiences and high levels of student engagement in community medicine education. Examination results provide contextual information on knowledge acquisition but may not fully reflect collaborative and creative competencies emphasized in the co-creation process. These findings suggest that student co-creation is a feasible pedagogical approach in community-oriented medical education, while highlighting the need for future research that uses aligned assessment strategies and more robust study designs.
Downloads
Metrics
References
Bovill C, Cook‐Sather A, Felten P. Students as co‐creators of teaching approaches, course design, and curricula: implications for academic developers. Int J Acad Dev 2011; 16: 133-45. DOI: https://doi.org/10.1080/1360144X.2011.568690
Cook-Sather A, Bovill C, Felten P. Engaging students as partners in learning and teaching: a guide for faculty. First edition. San Francisco: Jossey-Bass; 2014. 269 p. (The Jossey-Bass Higher and Adult Education Series).
Dollinger M, Lodge J, Coates H. Co-creation in higher education: towards a conceptual model. J Mark High Educ 2018; 28: 210–31. DOI: https://doi.org/10.1080/08841241.2018.1466756
Freitas FA, Leonard LJ. Maslow’s hierarchy of needs and student academic success. Teach Learn Nurs 2011; 6: 9-13. DOI: https://doi.org/10.1016/j.teln.2010.07.004
Bovill C, Cook-Sather A, Felten P, Millard L, Moore-Cherry N. Addressing potential challenges in co-creating learning and teaching: overcoming resistance, navigating institutional norms and ensuring inclusivity in student–staff partnerships. High Educ 2016; 71: 195-208. DOI: https://doi.org/10.1007/s10734-015-9896-4
Könings KD, Mordang S, Smeenk F, Stassen L, Ramani S. Learner involvement in the cocreation of teaching and learning: Amee guide no. 138 Med Teach 2021; 43: 924-36.
Noosen P, Rangkrut S. The need for faculty development in medical education in Thai medical lecturers. Siriraj Med Bull 2021; 14: 13–20.
Wallerstein NB, Duran B. Using communitybased participatory research to address health disparities. Health Promot Pract 2006; 7: 312–23. DOI: https://doi.org/10.1177/1524839906289376
Negandhi H, Sharma K, Zodpey SP. How can Departments of Community Medicine shape the future of public health education in India? Indian J Public Health 2010; 54: 184. DOI: https://doi.org/10.4103/0019-557X.77257
Papa R, Sixsmith J, Giammarchi C, Lippke S, McKenna V, Di Furia L, et al. Health literacy education at the time of COVID-19: Development and piloting of an educational programme for university health professional students in 4 European countries [Internet]. U.S. National Library of Medicine; 2023 DOI: https://doi.org/10.1186/s12909-023-04608-3
Kempster C, Gray J, Burman K. Studentdriven partnerships enhancing oral health literacy. Health Promot J Austr .2021; 32 Suppl 1: 98–103. DOI: https://doi.org/10.1002/hpja.376
Könings KD, Mordang S, Smeenk F, Stassen L, Ramani S. Learner involvement in the co-creation of teaching and learning: AMEE Guide No. 138. Med Teach 2021 Sep 30] from: https://www.tandfonline.com/doi/abs/10.1080/0142159X.2020.1838464 DOI: https://doi.org/10.1080/0142159X.2020.1838464
Adam AM. Sample size determination in survey research. J Sci Res Rep 2020; 90-7. DOI: https://doi.org/10.9734/jsrr/2020/v26i530263
Liu K, Liu S, Ma Y, Jiang J, Liu Z, Wan Y. Comparison of blended learning and traditional lecture method on learning outcomes in the evidence-based medicine course: a comparative study. BMC Med Educ 2024; 24: 680. DOI: https://doi.org/10.1186/s12909-024-05659-w
Ambrosetti É, Gaudin C, Flandin S, Poizat G. Students as co-designers in health professional education: a scoping review. BMC Med Educ 2025; 25: 645. DOI: https://doi.org/10.1186/s12909-025-07110-0
Killam LA, Egan R, Godfrey C, Ross-White A, Camargo-Plazas P, Lock M, et al. PROTOCOL: Learner-educator co-creation of student assessment in health professional education courses: A scoping review protocol. Campbell Syst Rev 2024; 20: e1392. DOI: https://doi.org/10.1002/cl2.1392
Rae VI, Smith SE, Hopkins SR, Tallentire VR. From corners to community: exploring medical students’ sense of belonging through co-creation in clinical learning. BMC Med Educ 2024; 24: 474. DOI: https://doi.org/10.1186/s12909-024-05413-2
Fakoya J, Ndrio M, McCarthy K. Facilitating active collaborative learning in medical education; a literature review of peer instruction method. Adv Med Educ Pract 2023;14: 1087–99. DOI: https://doi.org/10.2147/AMEP.S421400
Jeevan Divakaran. Active learning in medical education: A brief overview of its benefits. MARPAT 2025; 2: 4
Müller AM, Ngiam NSP, Dunn M, Samarasekera DD, Goh BYS, Goh CEH, et al. Developing empathy in healthcare professions students: protocol of a mixed-methods non-controlled longitudinal intervention study. Front Med 2024; 11: 2024. DOI: https://doi.org/10.3389/fmed.2024.1452516
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Journal of Southeast Asian Medical Research

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
The Journal of Southeast Asian Medical Research will hold the copyright to all published articles. The publisher's production department handles copyright forms once a manuscript is accepted and scheduled for publication.







